What is the Global Revenue Cycle Management Market Size?
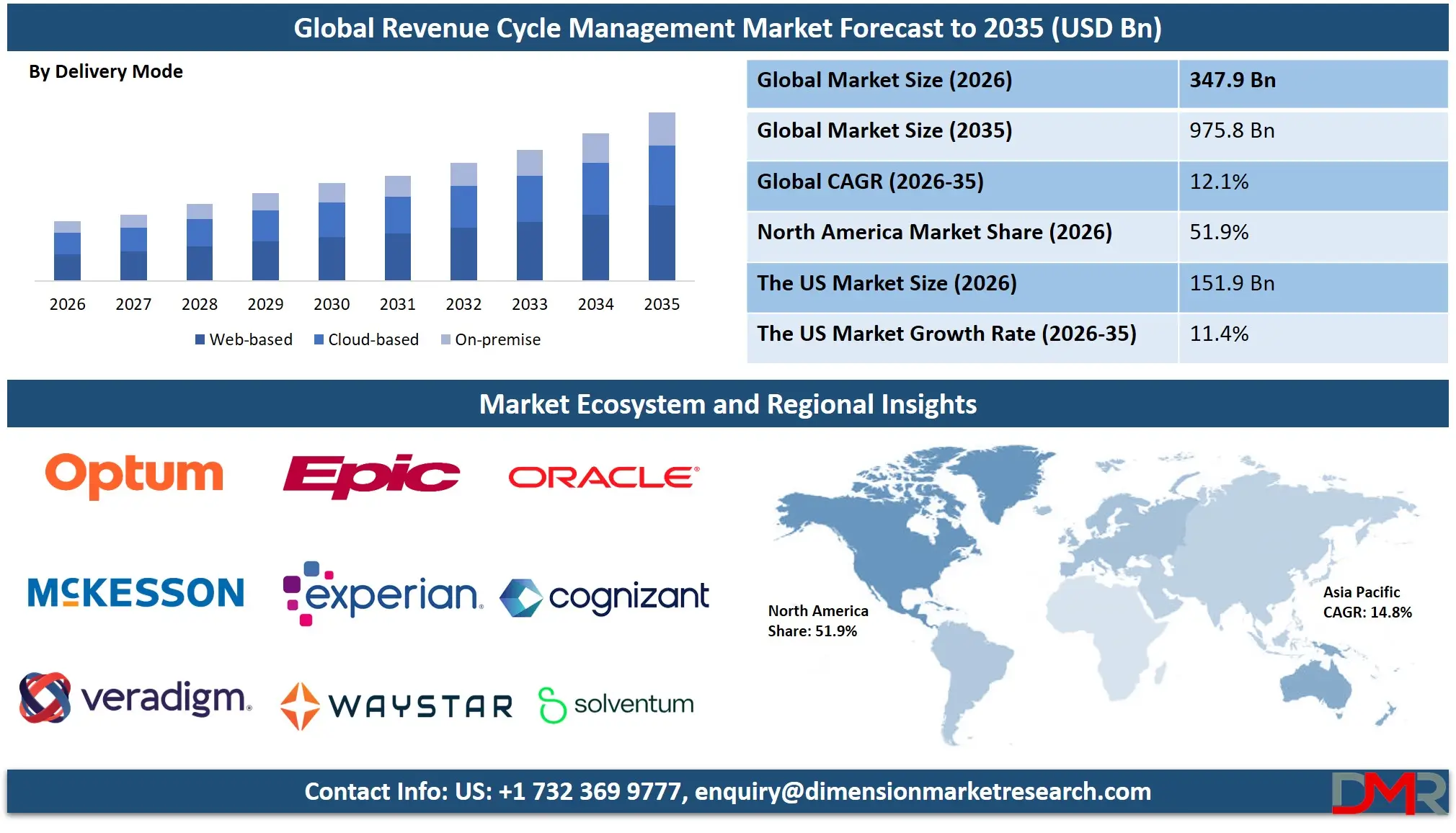
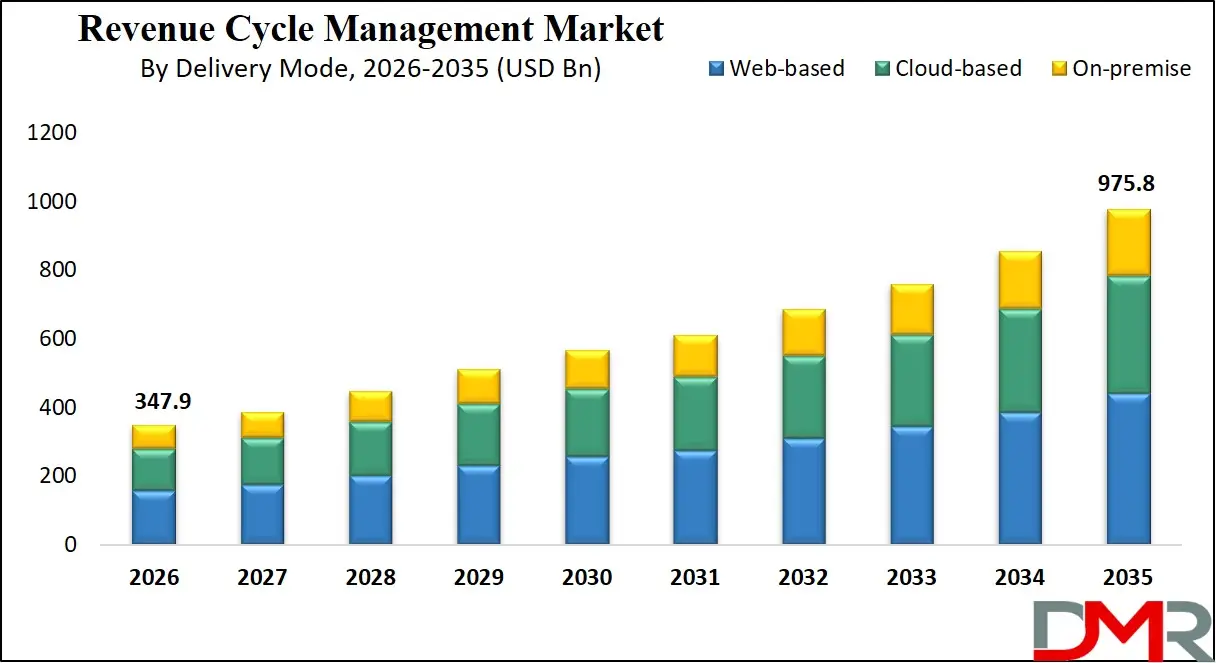
The Global Revenue Cycle Management Market size is estimated at USD 347.9 billion in 2026 and is projected to reach USD 975.8 billion by 2035, exhibiting a CAGR of 12.1% during the forecast period, driven by the growing adoption of automation, AI-enabled analytics, and integrated end-to-end RCM workflows in healthcare financial operations.
ℹ
To learn more about this report –
Download Your Free Sample Report Here
The growth of the Revenue Cycle Management (RCM) market can be attributed to the increased use of automation and artificial intelligence in claims processing and denial management, regulatory pressure to enhance transparency and decrease the number of errors within the billing process, and significant investment in technology infrastructure.
Other elements that contribute to market growth are advances in denial reduction predictive analytics, automation of medical coding, enhanced EHR and billing software integration, and increased demand for effective revenue management from healthcare providers. Digital transformation within the areas of billing, coding, and patient access has enabled great progress in the industry through improving efficiencies and decreasing claim denials while decreasing the cycle time.
ℹ
To learn more about this report –
Download Your Free Sample Report Here
The US Revenue Cycle Management Market
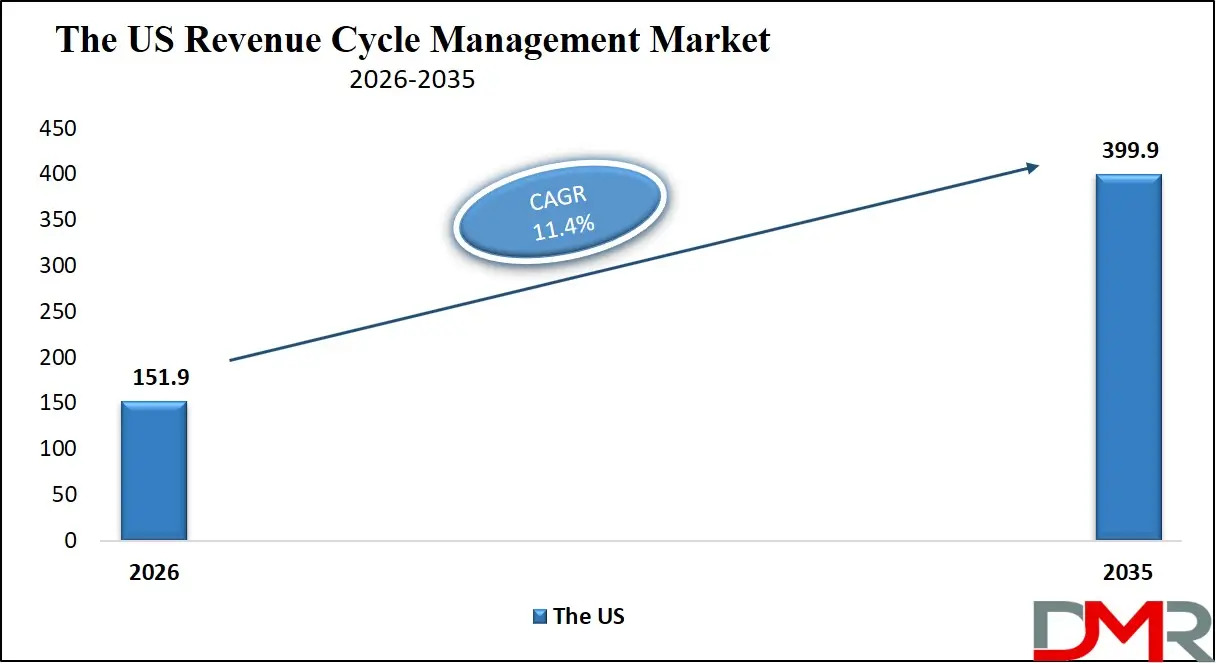
The US Revenue Cycle Management Market is estimated to grow to USD 151.9 billion in 2026 with a compound annual growth rate of 11.4% during the forecast period.
ℹ
To learn more about this report –
Download Your Free Sample Report Here
The US market is driven by powerful regulatory frameworks, including CMS reimbursement policies, HIPAA compliance requirements, and shift to value-based care models, focusing on efficiency, transparency, and better patient outcomes. Automated RCM solutions are becoming widely used by healthcare providers in an effort to handle complicated billing programs, minimize administrative loads and enhance financial results. The availability of advanced healthcare IT infrastructure, the popularity of the use of EHR systems, and the emphasis on interoperability also contribute to the market growth. Moreover, the RCM services outsourcing trend is becoming popular among hospitals and physician groups that aim to optimize costs and ensure operational efficiency.
Europe Revenue Cycle Management Market
The Europe Revenue Cycle Management Market is estimated to be valued at USD 100.4 billion in 2026, witnessing growth at a CAGR of 11.2%, during the forecast period.
The European market is characterized by tough regulatory standards, the growing attention to healthcare cost optimization, and the growth in the use of digital health solutions. RCM is being adopted with the assistance of government efforts to facilitate the digitization of healthcare and the interoperability of cross-border data. Germany, France, and the UK are some of the countries that are investing in healthcare IT systems to enhance billing efficiency and minimize administrative expenses. Moreover, the increasing pressure to comply with regional data protection laws and enhance reimbursement procedures is also promoting the usage of advanced RCM solutions. Public-private partnerships and rising investments in healthcare digital transformation further support the market.
Japan Revenue Cycle Management Market
The Japan Revenue Cycle Management Market is projected to be valued at USD 10.1 billion in 2026, progressing at a CAGR of 13.9%, during the period spanning from 2026 to 2035.
Japan's RCM market is also conditioned by well-developed healthcare facilities, growing use of automatization technologies, and the tendency to pay much attention to the efficiency of operations. The aging population and increased healthcare need in the country is fueling the necessity to have efficient billing and reimbursement systems. The market is further being facilitated by government efforts to encourage digital health change and use of the healthcare IT. Moreover, healthcare providers are turning to AI and analytics to enhance the accuracy of claims, minimize denials, and increase efficiency in the revenue cycle.
Key Takeaways
- Market Size & Forecast: The Global Revenue Cycle Management Market is estimated to be valued at USD 347.9 billion in 2026 and is expected to grow to USD 975.8 billion by 2035.
- Growth Rate & Outlook: The market is expected to witness growth at a compound annual growth rate of 12.1% in the forecast period.
- Primary Growth Drivers: Increasing adoption of automation and AI in claims management, regulatory compliance requirements, and growing healthcare IT investments are some of the key drivers of growth in the market.
- Key Market Trends: Shift toward cloud-based RCM solutions, predictive analytics for denial management, and outsourcing of revenue cycle functions are the key trends in the market.
- By Component: The Software segment is anticipated to get the majority share of the RCM market in 2026.
- By Delivery Mode: The Cloud-based segment is expected to occupy the largest revenue share in 2026 in the RCM market.
- By End User: Hospitals are predicted to dominate the market in 2026, with high patient volumes and complex billing workflows.
- Regional Leadership: North America is predicted to dominate the market with an estimated 51.9% share in 2026, with high healthcare digital transformation spend and RCM technology investment.
What is Revenue Cycle Management?
Revenue Cycle Management (RCM) is a term used to describe the financial process that healthcare organizations use to administer and clinically coordinate their services from the point of registration of the patient up until payment and revenue collection. The RCM involves patient registration, insurance verification, medical coding, billing, claims submission, payments, and denial management.
Use Cases
- Claims Submission for Commercial Payers: RCM platforms are capable of generating high-volume claim structures in real-time to discover optimal billing configurations for commercial insurers, Medicare, and Medicaid with turnaround times on the order of days, saving orders of magnitude over time compared with manually submitting claims from templates.
- Payment Obligation & Denial Optimization: Long-term payment performance and denial data, such as appeal success rates and reimbursement delays, are modeled to give risk mitigation recommendations and keep safely managing revenue portfolios without disruption to ensure operational stability and revenue confidence.
- Compliance Monitoring & Control: Enterprise deployments are employing machine learning and claims analytics to perform real-time denial prediction, compliance anomaly detection, and automated alert adjustment with quantifiable and proven accuracy.
- Population Health & Government Programs: More efficient RCM systems contribute to the success of public healthcare reimbursement, regulatory compliance in Medicare/Medicaid, and smart claims surveillance, facilitate national digital health adoption, contribute to deployment reliability, and help implement policies such as data governance policy and digital claims standards.
How AI Is Transforming the Global Revenue Cycle Management Market?
AI has transformed the realm of RCM, providing the potential for modeling how likely claims will be approved and get reimbursed, as well as recognizing anomalies in the billing process and optimizing various parameters for billing in different departments in health organizations. Claims and operational data can be analyzed through an AI-based model to detect issues related to compliance, proper coding, and inefficient workflows that will lead to optimization of revenues. This approach offers savings in terms of both time and effort needed to conduct such analyses manually.
Furthermore, intelligent workflow scheduling, predicting any risk to claims approvals, and prioritization of tasks become possible thanks to AI applications in the revenue cycle management area. It also makes it easier for healthcare facilities to cut costs related to manual reviews and performance monitoring, thereby streamlining operations and minimizing expenses.
Market Dynamics
Key Drivers of the Global Revenue Cycle Management Market
AI-Driven Claims Intelligence and Real-Time Analytics
The market is being pushed by a fast uptake of AI-driven claims denial and payment obligation optimization, high-efficiency claims data processing, API-based interoperability with EHR and practice management systems, and real-time analytics from claims repositories. These technologies enable monitoring of the performance of RCM systems in real time, identify compliance anomalies early, predict denial rates, and simplify the process of payment validation. Consequently, operational uptime and departmental efficiency are highly enhanced while minimizing the costs of manual data analysis. The growth of machine learning models for billing optimization, in particular, is also accelerating the need for intelligent RCM automation, as healthcare operators are increasingly adopting automation and workflow optimization based on claims payment performance data.
Rising Regulatory Compliance Requirements
The world is increasingly focused on claims security and quality, with governments and regulatory bodies introducing digital claims efficiency frameworks, such as the EU Digital Single Market provisions for health data and the US CMS's digital reporting frameworks for Medicare and Medicaid claims. These structures are driving demand for efficient RCM automation capable of supporting real-time compliance monitoring and continuous learning. In parallel, global initiatives promoting claims standardization and workforce development are encouraging the adoption of evidence-based RCM architectures. The increasing focus on transparency in claims design and reduction in denial rates is also enhancing the necessity of reliable and scalable RCM automation in both public and private healthcare systems.
Restraints in the Global Revenue Cycle Management Market
High Integration and Validation Costs
RCM platforms are expensive and time-intensive to implement, need to be heavily tested in healthcare settings, and process logic reliability is tested, and long-term performance evaluation of new components is needed. Also, regulatory limitations and data privacy regulations (e.g., HIPAA for claims data, patient protections) add to the complexity and cost of deployment. These aspects pose barriers to entry, lengthen deployment, and raise initial capital investments.
Lack of Standardization Across RCM Systems
The industry continues to rely on multiple RCM automation architectures, including rules-based, AI-based for denial optimization, and NLP-based for code extraction. However, the lack of standardized claims data interfaces beyond platforms like Epic and Cerner remains a key challenge. RCM lacks universal plug-and-play standards compared to traditional EHR modules, making integration complex and limiting interoperability of RCM models across different hospital billing, physician practice, and revenue integrity systems.
Growth Opportunities in the Global Revenue Cycle Management Market
Expansion in Emerging Digital Health Markets
Developing digital health markets such as Brazil, Indonesia, Nigeria, the UAE, and Vietnam are investing in digital health infrastructure and advanced RCM capabilities. These regions present strong growth potential due to increasing demand for automated claims generation, compliance monitoring, and remote billing consultation applications. With limited legacy revenue infrastructure, they provide opportunities for the deployment of modern RCM automation optimized for healthcare financial environments.
Growing Shift Toward Cloud-Based RCM Solutions
The increased requirement for advanced RCM automation is being generated by the growth of remote healthcare collaboration, distributed hospital operations, and real-time revenue control applications. These technologies play a vital role in virtual RCM platforms, remote billing operations, and digital health innovation hubs. With the rising importance of sub-hour claims processing as a major operational concern, cloud-based RCM analytics capabilities are likely to be fundamental to future healthcare and digital health IT infrastructure.
Global Revenue Cycle Management Market Trends
Increasing Adoption of Predictive Denial and Analytics
RCM platforms are being monitored and process logic anomalies are detected in real time, and payment override patterns are predicted using on-system learning. The use of digital twin models of claims risk and machine learning algorithms is enhancing claims workflow scheduling, system lifespan, and deployment reliability. This shift is transforming RCM management from manual data review to a fully automated, continuously optimized system monitoring.
Cloud-Based Revenue Monitoring and Management
Cloud computing and digital twin technologies are taking centre stage in the operations of RCM deployments. These platforms enable real-time storage and analysis of claims payment performance data, centralized portfolio management of automated workflows, and remote monitoring of RCM module health. Cloud-based systems enhance transparency, lower on-prem infrastructure expenses, and provide quicker responses to workflow changes across hospital sites, as experienced by operators of large RCM networks.
Research Scope and Analysis
The global Revenue Cycle Management market is witnessing strong growth across services, integrated platforms, cloud deployment, outsourced operations, and hospital-based adoption. Increasing demand for workflow automation, AI-enabled claims management, and seamless EHR integration continues to enhance operational efficiency, reimbursement accuracy, and healthcare financial performance.
ℹ
To learn more about this report –
Download Your Free Sample Report Here
By Component Analysis
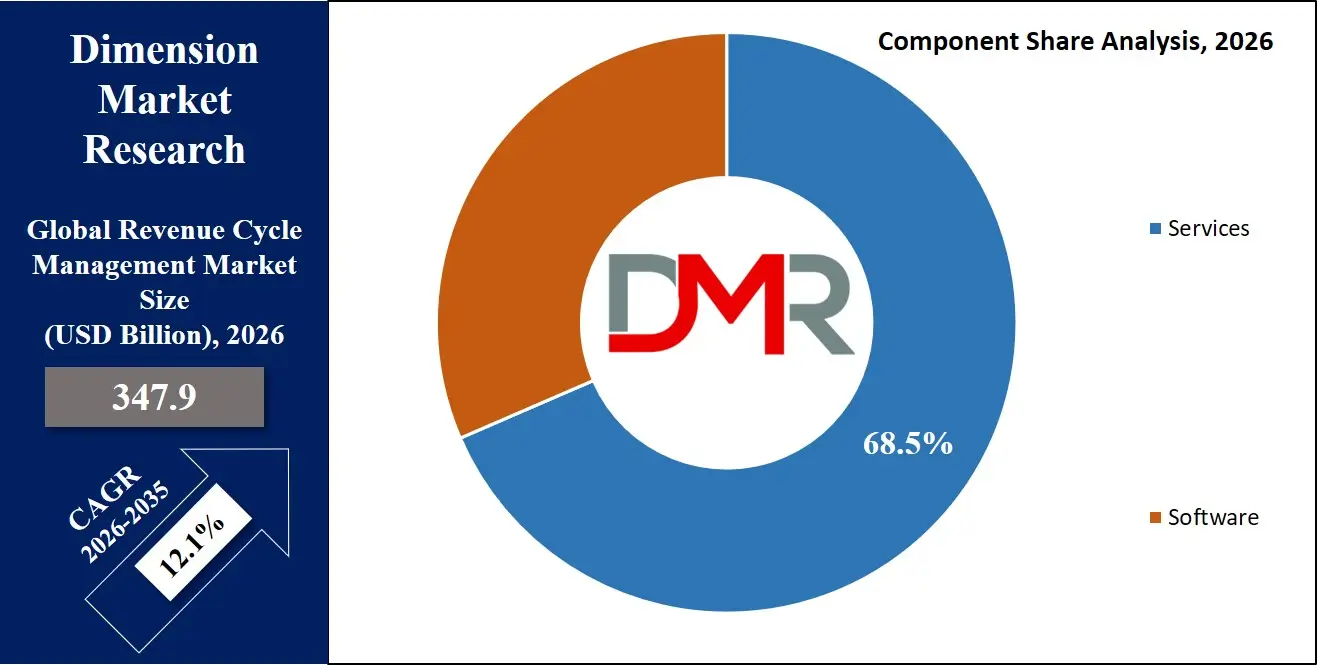
The Services segment is expected to remain the largest in 2026, accounting for about 68.5% share of the global RCM market, driven by its dominant use in large-scale revenue portfolio management, seamless EHR/practice management workflow integration, and flexibility across diverse healthcare frameworks where real-time claims data access and service ecosystem maturity are essential. Meanwhile, the Software segment is witnessing strong growth, driven by rising demand for deployment, integration, training, and support solutions in healthcare settings where real-time data capture and process efficiency are critical. Adoption is further supported by workflow optimization, real-time efficiency improvements, and modular configurations that integrate multiple process capabilities for improved workflow flexibility and user satisfaction.
By Type Analysis
The Integrated segment is expected to account for the largest share in 2026 with around 66.4% share, as healthcare enterprises heavily rely on integrated RCM platforms that seamlessly connect with EHR and practice management systems for claims submission, payment posting, and denial tracking. The segment is further supported by increasing deployment of AI-enabled claims analytics, automated denial management systems, and integrated workflow platforms that enhance process reproducibility and operational efficiency across hospital billing, coding, and revenue integrity applications. The Standalone segment remains relevant for smaller practices and clinics that require focused functionality without full enterprise integration, particularly in ambulatory and diagnostic lab settings.
By Delivery Mode Analysis
The Cloud-based segment is expected to account for the largest share in 2026 with around 55.2% share, as healthcare providers increasingly rely on cloud RCM platforms for claims storage, approval workflows, and compliance tracking. The segment is further supported by increasing deployment of AI-enabled claims analytics, automated denial systems, and integrated workflow platforms that enhance process reproducibility and operational efficiency across hospital billing and physician practice applications. It is also among the fastest-growing segments in the RCM market. The Web-based segment offers accessibility without installation, popular among smaller end users. The On-premise segment remains relevant for large hospital systems with strict data sovereignty, security requirements, and legacy EHR integrations.
By Sourcing Analysis
The Outsourced RCM segment is expected to dominate with an estimated 58.3% share in 2026, driven by healthcare providers' focus on core clinical operations, rising complexity of payer requirements, and the need for specialized revenue expertise without extensive in-house infrastructure. The In-house RCM segment remains significant for large health systems and hospitals with sufficient capital and staffing to manage revenue operations internally, offering greater direct control over patient financial interactions and claims workflows.
By Function Analysis
The Claims and Denial Management segment is expected to dominate with around 32.5% share in 2026, driven by the critical need for rapid and accurate claims submission, denial tracking, appeal management, and reimbursement optimization. The Coding and Billing segment follows closely, utilizing RCM for accurate medical code assignment and charge capture. Patient Access is witnessing strong growth as organizations seek to streamline registration, eligibility verification, and prior authorization. Clinical Documentation, Revenue Integrity, and Payment Processing segments are also adopting RCM solutions to ensure compliance, reduce manual effort, and improve revenue capture across healthcare functions.
By End User Analysis
The Hospitals segment represents the largest share in 2026, accounting for an estimated 48.6% of the market, driven by high patient volumes, complex billing workflows, and the need for advanced compliance and integration capabilities with EHR systems. Hospitals benefit from dedicated billing, coding, and revenue integrity teams that can fully utilize enterprise-grade RCM platforms. The Physician Offices & Clinics segment is the fastest-growing, as cloud-based, subscription-friendly RCM solutions become more accessible, affordable, and easier to deploy without extensive IT resources. Diagnostics Labs and Other end users (including ambulatory surgery centers and nursing homes) are increasingly adopting RCM to digitize billing processes, reduce claim denials, and improve operational efficiency.
The Global Revenue Cycle Management Market Report is segmented based on the following:
By Component
By Type
By Delivery Mode
- Web-based
- Cloud-based
- On-premise
By Sourcing
- In-house RCM
- Outsourced RCM
By Function
- Claims and Denial Management
- Coding and Billing
- Patient Access
- Clinical Documentation
- Revenue Integrity
- Payment Processing
By End User
- Physician Offices & Clinics
- Hospitals
- Diagnostics Labs
- Others
Regional Analysis
Leading Region in the Revenue Cycle Management Market
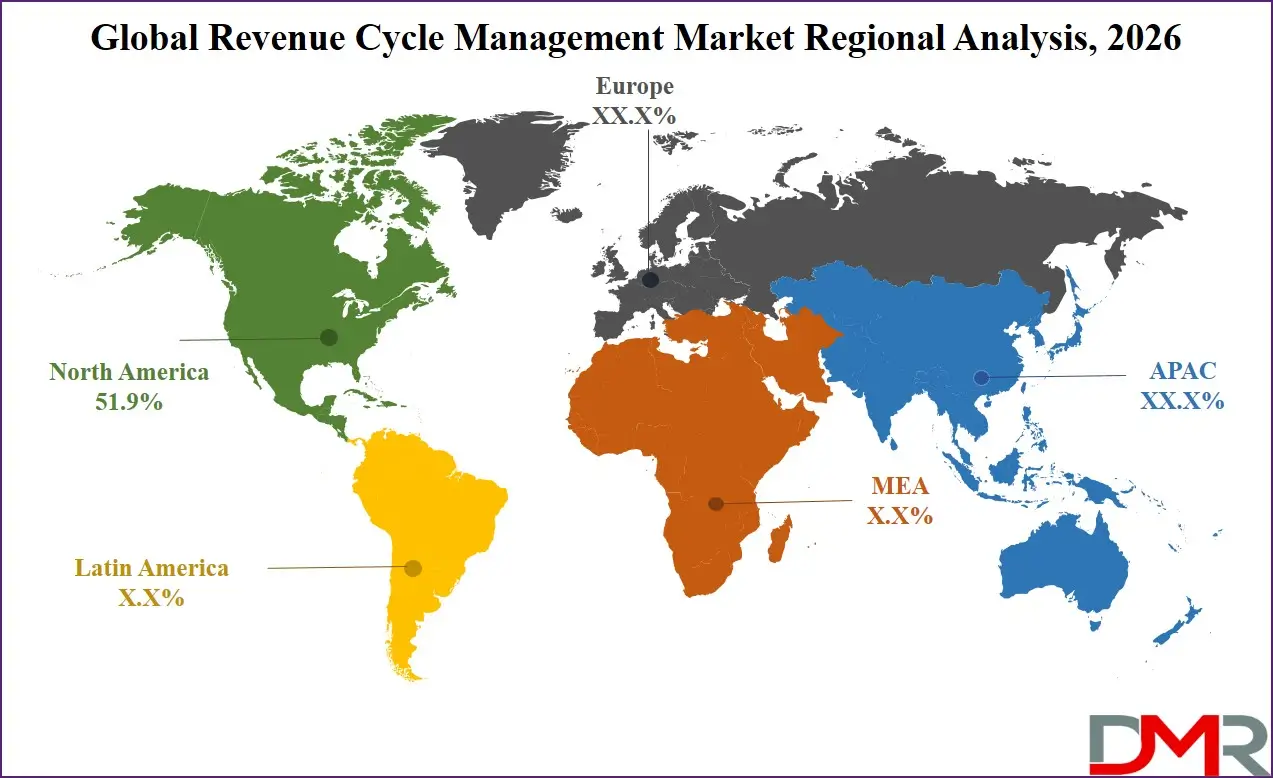
It is projected that North America will take the lead in the global RCM market (by value), covering a market share of about 51.9% in the year 2026. The region's dominance is driven by strong healthcare digital transformation cadence (US-based National AI in Healthcare Billing Initiative and NIST digital claims programs), high software and services prices relative to other regions, a mature healthcare IT supply chain for advanced interoperability and high-speed data exchange, and the presence of key RCM vendors and digital transformation consultancies. The widespread adoption of advanced machine learning and workflow-based RCM automation for hospital billing, physician coding, and revenue compliance further strengthens North America's leading position in the market. Additionally, continuous investments in AI-enabled process logic monitoring and interoperability capabilities are further reinforcing regional technological leadership.
ℹ
To learn more about this report –
Download Your Free Sample Report Here
Fastest-Growing Region in the Revenue Cycle Management Market
Asia-Pacific is the fastest-growing region, supported by strong digital transformation deployment targets (China, India, Japan), increasing data sovereignty initiatives, rising investments in domestic RCM capabilities, and growing adoption of automated revenue management systems. The region benefits from well-established IT services capacity for automated workflows, increasing commercial participation, and alignment with national digital health roadmaps. Countries across the region are actively deploying RCM to enhance operational productivity-per-dollar and strengthen healthcare digital infrastructure. Growing emphasis on RCM R&D and structured process logic development further accelerates market expansion in the region. Moreover, increasing government support and commercial enterprise commitments are expected to sustain high growth momentum.
By Region
North America
Europe
- Germany
- The U.K.
- France
- Italy
- Russia
- Spain
- Benelux
- Nordic
- Rest of Europe
Asia-Pacific
- China
- Japan
- South Korea
- India
- ANZ
- ASEAN
- Rest of Asia-Pacific
Latin America
- Brazil
- Mexico
- Argentina
- Colombia
- Rest of Latin America
Middle East & Africa
- Saudi Arabia
- UAE
- South Africa
- Israel
- Egypt
- Rest of MEA
Competitive Landscape
The RCM market is highly competitive, with innovation and strategic alliances shaping the competitive environment. In order to achieve a competitive advantage, companies are focused on the development of advanced automation capabilities (e.g., AI-based denial management, workflow automation for claims processing, and machine learning for revenue optimization), AI-powered claims analytics, and compliance monitoring solutions. There are high barriers to entry due to capital-intensive implementation requirements, specialized healthcare billing and compliance expertise, and the need for mature software ecosystems and adherence to healthcare regulatory and payer requirements.
Strategic approaches in the market to increase market presence include partnerships with hospitals and digital health providers, mergers between RCM solution providers and healthcare IT companies, and long-term service contracts with billing departments, revenue integrity teams, and academic medical institutions. Moreover, research and development in interoperability frameworks and scalable software platforms are important factors in maintaining competitiveness and addressing the evolving needs of the healthcare industry.
Some of the prominent players in the Global Revenue Cycle Management Market are:
- Optum, Inc.
- Epic Systems Corporation
- Oracle Corporation
- R1 RCM Inc.
- McKesson Corporation
- athenahealth, Inc.
- Conifer Health Solutions, LLC
- Experian Information Solutions, Inc.
- Cognizant Technology Solutions Corporation
- eClinicalWorks, LLC
- Veradigm LLC
- GeBBS Healthcare Solutions, Inc.
- NextGen Healthcare, Inc.
- CareCloud, Inc.
- Waystar, Inc.
- Medical Information Technology, Inc.
- FinThrive, Inc.
- Solventum Corporation
- The SSI Group, LLC
- Omega Healthcare Management Services Private Limited
- Other Key Players
Recent Developments
- March 2026: Optum, Inc. partnered with Microsoft to enhance AI-driven claims processing and reimbursement workflows, leveraging real-time data integration to improve transparency and efficiency in revenue cycle operations.
- October 2025: Ensemble Health Partners engaged JPMorgan and Goldman Sachs to explore a potential USD 13 billion sale or IPO, reflecting strong investor interest in AI-enabled revenue cycle management platforms and large-scale outsourcing models.
- May 2025: Infinx expanded its global RCM capabilities through the acquisition of the healthcare revenue cycle business of i3 Verticals for USD 96.0 million, strengthening its presence in the US healthcare systems and enhancing its technology portfolio.
- October 2024: Oracle Health announced the general availability of its next-generation Revenue Cycle Management platform, built on Oracle Cloud Infrastructure, integrating AI-driven claims management capabilities, real-time data workflows, and enhanced patient access-to-payment automation, strengthening its enterprise RCM and EHR ecosystem.
Report Details
| Report Characteristics |
| Market Size (2026) |
USD 347.9 Bn |
| Forecast Value (2035) |
USD 975.8 Bn |
| CAGR (2026–2035) |
12.1% |
| The US Market Size (2026) |
USD 151.9 Bn |
| Historical Period |
2021 – 2025 |
| Forecast Period |
2027 – 2035 |
| Base Year |
2025 |
| Estimated Year |
2026 |
| Segments Covered |
By Component (Services, Software), By Type (Integrated, Standalone), By Delivery Mode (Web-based, Cloud-based, On-premise), By Sourcing (In-house RCM, Outsourced RCM), By Function (Claims and Denial Management, Coding and Billing, Patient Access, Clinical Documentation, Revenue Integrity, Payment Processing), By End User (Physician Offices & Clinics, Hospitals, Diagnostic Labs, Others) |
| Regional Coverage |
North America – The US and Canada; Europe – Germany, The UK, France, Russia, Spain, Italy, Benelux, Nordic, & Rest of Europe; Asia-Pacific – China, Japan, South Korea, India, ANZ, ASEAN, Rest of APAC; Latin America – Brazil, Mexico, Argentina, Colombia, Rest of Latin America; Middle East & Africa – Saudi Arabia, UAE, South Africa, Turkey, Egypt, Israel, & Rest of MEA |
Frequently Asked Questions
How big is the Global Revenue Cycle Management Market?
▾ The Global Revenue Cycle Management Market size is estimated to have a value of USD 347.9 billion in 2026 and is expected to reach USD 975.8 billion by the end of 2035.
Which region held the largest share of the Global Revenue Cycle Management Market in 2026?
▾ North America is expected to account for the largest market share in 2026, with a share of about 51.9%.
Who are the key players in the Global Revenue Cycle Management Market?
▾ Some of the major key players in the Global Revenue Cycle Management Market are Epic Systems Corporation, McKesson Corporation, Change Healthcare, Inc., R1 RCM Inc., Optum, Inc., and many others.
What is the CAGR of the Global Revenue Cycle Management Market from 2026 to 2035?
▾ The market is growing at a CAGR of 12.1% over the forecasted period.
What factors are driving the growth of the Global Revenue Cycle Management Market?
▾ The market is driven by advances in machine learning-based claims denial and reimbursement optimization, regulatory pressure to accelerate claims approvals and reduce denial rates, and increasing government investment in national digital health infrastructure.
What are the major trends in the Global Revenue Cycle Management Market?
▾ The key market trends include the adoption of predictive denial outcome monitoring and real-time payment control, along with a growing shift toward cloud-based RCM platforms and analytics-enabled workflow management systems.
Which region is expected to grow the fastest in the Global Revenue Cycle Management Market?
▾ Asia Pacific is the fastest-growing region in the market during the forecast period.
How is the Global Revenue Cycle Management Market segmented?
▾ The market is segmented by component, type, delivery mode, sourcing, function, and end user.